We get a ton of emails and visits from people wanting to get off blood thinners after a stent. People are not satisfied with the typical cardiologist’s recommendation, ” Stay on them for life.”
I am not satisfied with that answer and you shouldn’t be either. We can do better.
In this post, I will discuss:
If an angiogram was performed, and one or more blockages were found, the cardiologist determined that one or more stents would be beneficial.
A stent is a metal device that keeps arteries open after an angioplasty. Angioplasty was the first intravascular (inside the artery) therapy to open a blood vessel using a balloon over a wire inserted into the vessel. Unfortunately, opening with a balloon led to many failures in the short-term with the sudden closure of the artery and in the long-term with a repeat blockage in the same area called a re-occlusion.
Stents were developed to limit the short-term sudden closure. But first-generation stents led to scar tissue, that over time, led to a repeat blockage. Second generation stents were then coated with chemotherapy drugs to limit scar tissue formation.
To prevent sudden blockage after a stent, aspirin and a more advanced platelet blocker was added. Platelets are part of the blood clotting system that aspirin works on. These have brand names like Plavix, Brilinta, and Effient. Together, aspirin and one of these agents is called DAPT, or Dual Anti-Platelet Inhibitor Therapy.
The longer the duration of the DAPT, the less likely the stents will shut down. This can be good. But these are heavy-duty blood thinners that can lead to much higher bleeding rates.
So, the question becomes one of risk versus benefit. What is the risk of a major bleed versus the risk of a stent shutting down? Both events can be catastrophic and life-threatening.
Many studies have assessed the optimal duration of DAPT. Again, the studies look at bleeding risk versus sudden-blockage risk, otherwise known as acute stent thrombosis.
I wrote a blog in 2015 discussing a trial reported in the British Medical Journal. At that time, a meta-analysis looked at 10 randomized trials with over 32,000 patients. Short term dual antiplatelet therapy (DAPT) was associated with less bleeding and NO INCREASE IN HEART ATTACKS compared with 12 months of therapy. Short term therapy is roughly defined as around 6 months.
The authors also looked at long term dual antiplatelet therapy greater than 12 months. When DAPT was continued longer than 12 months, heart attacks were less likely. Sounds good so far.
The bad news is that major bleeds were 62% more common and the death rate was 30% higher!
A calculator was produced a couple of years ago and points are awarded for risk factors. The more risk factors, the more points, and the higher the risk of the stent shutting down. Less of these risk factors meant that the risk of bleeding is too high, and the duration of DAPT should be shorter.
Here are the risk factors in the calculator:
Other factors in the DAPT score to be considered that increase the risk of thrombosis include whether this event was during a heart attack (versus elective and lower risk), smaller stent size, and stenting an older bypass graft.
The DAPT calculator can be found here. I have taken a screenshot so you can see what it looks like.
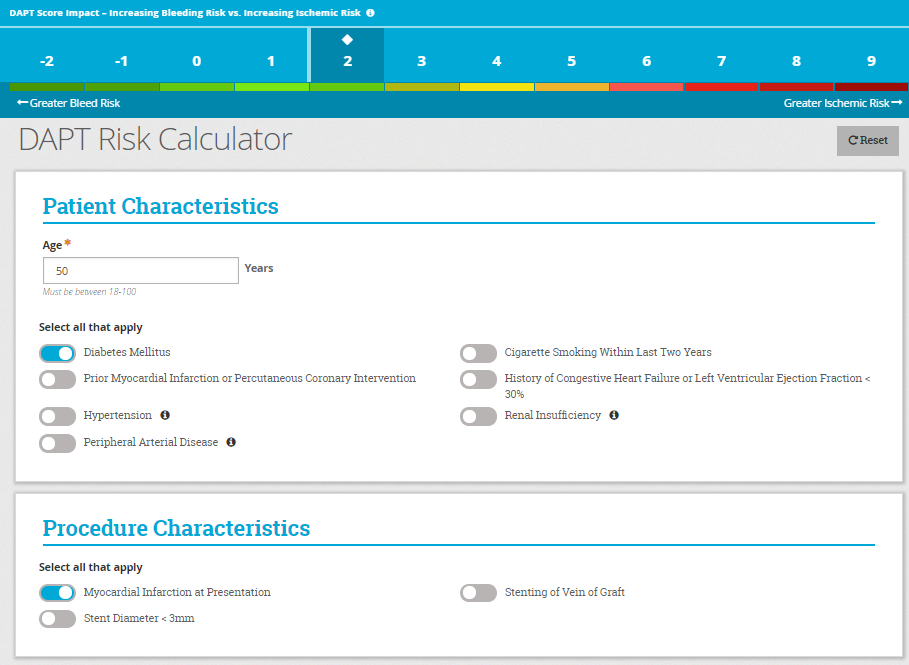
If the score is in the green territory from -2 to 3, 6 months of DAPT is appropriate. 4 and above should receive at least 12 months of DAPT or longer. Those people at 4 and above are at a much higher risk of the stent shutting down.
I have a different approach to the above plan. It is based on the fact that in our office we work to make you much healthier than the people in the studies that led to the creation of the DAPT score. Let’s face it. The people in the studies LIKELY do not eat well and do not follow a healthy lifestyle. You can imagine that ice cream eaters who have lousy sleep habits, are couch potatoes, and don’t get much sun are at higher risk than our mythical “Paleo Person.”
So, follow me on this. 3-6 months of DAPT if your score is below 4, and 6-12 months if your score is 4 or above.
I think you are at a much lower risk of shutting down that stent if you follow the Paleo lifestyle. I discuss these topics in my book, The Paleo Cardiologist, The Natural Way to Heart Health. The following recommendations can be done with OR without DAPT.
Talk with your doctor to see if this plan is right for you OR come out to Arizona and we can talk about it.
If you are concerned about your health and well-being, we’ve got you covered! Schedule a FREE call with a Drs. Wolfson health coach and get the guidance you need. Just click HERE and pick your coach.
Become a Wolf Pack Insider for free and get access to our articles and guides to live healthy naturally, without sickness, disease or Big Pharma meds. You'll learn all about disease prevention, natural treatment remedies, tasty healthy foods and how to detox your life.
Please read the comment policy before replying to this post.